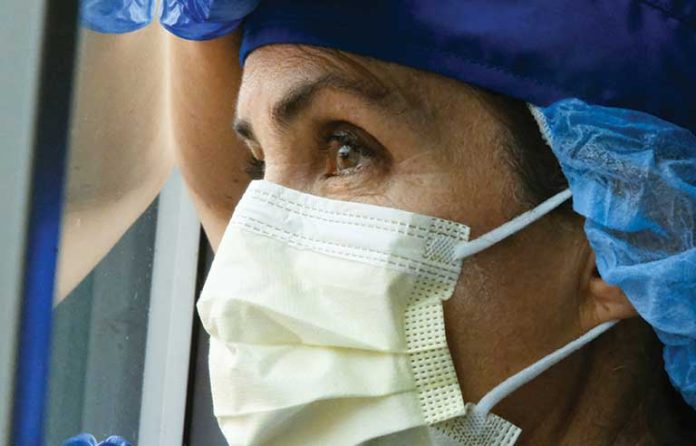
Toronto — Feelings of anxiety and depression were highest among workers whose perceived personal protective equipment and infection control needs were not met during the early months of the COVID-19 pandemic, according to the results of a recent study out of Canada.
The Institute for Work and Health, in partnership with the Occupational Health Clinics for Ontario Workers, from April 7 to May 13 conducted an online survey of nearly 6,000 health care professionals and more than 3,500 non-health care workers. The respondents were asked about the perceived need and adequacy of eight types of PPE and 10 different infection control practices on the job. The respondents’ associated anxiety and depression symptoms were assessed using the Generalized Anxiety Disorder (GAD-2) and Patient Health Questionnaire-2 screening tools, respectively.
Overall, 55% of the workers “screened positive” – scoring a three or higher on a six-point scale – for anxiety symptoms, while 42% screened positive for depression symptoms.
Less than 20% of the respondents had all their PPE or infection control needs met while working. Among those who had their workplace PPE needs fully met, 43% had GAD-2 scores of 3 or above. That increased to 60% among workers who felt none of their needs was being met.
PPE items mentioned in the survey were gloves, eye protection/goggles, faceshields, gowns, hand sanitizer, surgical/procedural masks, N95 respirators, and powered air-purifying respirators. The respondents also were asked about infection control practices such as screening incoming patients, having asymptomatic patients wear masks, restricted access and controlled flow of COVID-19 patients in a facility, ventilation, and cleaning/disinfection practices.
In a Nov. 4 press release, the researchers said strengthening employer-based infection control strategies has an important impact on the mental health of workers.
“Notably, people who felt fully protected at their worksites had similar or even slightly better mental health compared to people who worked from home,” the researchers said. “Likewise, people who felt entirely unprotected at work had even poorer mental health than people who had lost their jobs since the start of the pandemic.”
The study was published online Sept. 21 in the Canadian Journal of Psychiatry.